GRANTING SMILES Dental school gets $3.1 million grant to improve special needs care
The East Carolina University School of Dental Medicine has received a $3.1 million grant to enhance resident training in the care of patients with special needs in eastern North Carolina and across the state.
The award from the Health Resources and Services Administration, one of the largest in the dental school’s history, will focus on improving dental care for pediatric and elderly patients as well as those with mobility issues and other complex health problems and those with mental, emotional and behavioral challenges.

Members of the grant project team from the School of Dental Medicine and College of Allied Health Sciences meet via teleconference, led by principal investigator Dr. Michael Webb, right. (Photo by Jon Jones)
“This grant highlights our mission and strong community partnerships,” said Dr. Greg Chadwick, dean of the School of Dental Medicine. “It positions our residents and future dentists to work in rural communities and learn to engage and respond to patients’ complex health challenges.”
The five-year project, titled “ECU Leadership Training in Special Needs Population Oral Health Care,” will address three specific goals—assessing and treating the needs of vulnerable populations, expanding pediatric dentistry training to a rural location and developing tools and training for population health management.
“This project is intended to take dentists who have basic knowledge and skills in treating special populations and expand on these so that they are able to be leaders in the care of these patients,” said Dr. Michael Webb, principal investigator and chair of the School of Dental Medicine’s Department of Pediatric Dentistry and Orthodontics and Dentofacial Orthopedics.
Caring for special populations
The team will work to address three significant gaps in the current oral health care workforce, including the lack of readiness in treating children and adults with special health care needs.
According to the American Dental Education Association’s 2018 national Survey of Graduating Seniors, students expressed less confidence in their skills related to providing care for patients with physical, mental and developmental disabilities.
“This grant will allow the School of Dental Medicine to expand the scope of training for dental providers at all levels so that they are better prepared not only in the technical aspects of oral health care but also in working with community partners to provide total health care,” Webb said. “We are hoping to foster leadership skills in our residents so that they can extend this work beyond the time spent in the residency throughout their professional careers.”
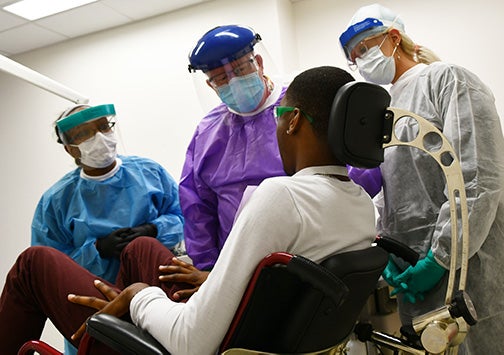
The grant, led by Dr. Michael Webb, center, will focus on improving resident education and dental care for patients with special health needs, including those treated in Ross Hall’s Special Needs Clinic, above. (Photo by Jon Jones)
The project will include academic input in the areas of pediatrics, nursing, pediatric dentistry, general dentistry and dental public health. Pediatric dentistry training will be expanded to a rural site in Hertford County. Residents from the existing Advanced Education in General Dentistry (AEGD) program will be offered a second year of training that emphasizes oral health care delivery for vulnerable populations.
According to data from the 2016 National Residential Information Systems Project, about 60% of people with intellectual and/or developmental disabilities are covered by Medicaid. Most dentists do not participate in Medicaid because reimbursement is low, which makes it difficult for these patients to get access to dental care, with little opportunity for prevention or early intervention. As a result, dental disease is more advanced and dental treatment needs are more complex.
Once the planning year is complete, the project will provide enhanced training to three residents per year. Trainees will be recruited from the existing programs that include 21 AEGD residents and six pediatric dentistry residents.
Providing dentists for rural North Carolina
The second gap in oral health care that the grant will help address is the shortage of dentists in rural and underserved areas of the state.
“Rural communities in North Carolina have a need for dentists, especially pediatric dentists,” Webb said, “who are part of a medical-dental health-care team that can address social determinants of health. Underserved populations including patients with special needs and those in rural communities have multiple barriers to care that need to be addressed.”
Those factors, the conditions in which people are born, grow, live, work and age, and can include socioeconomic status, education, neighborhood and physical environment, employment, social support networks, as well as access to health care, take interprofessional teams to address.
Also leading the project is Dr. Mark Moss, co-project director and associate professor in the dental school’s Department of Foundational Sciences. Other dental school team members include Dr. David MacPherson, clinical assistant professor and director of the AEGD program; Dr. Ford Grant, director of the school’s community service learning center in Ahoskie; Dr. Robert Carter Jr., director of the special care dentistry program; and Dr. Wanda Wright, assistant professor and division director of dental public health. Dr. Molly Jacobs, a health economist and assistant professor in health services and information management, represents the College of Allied Health Sciences.
“If you spend a little time here things start to make sense,” Moss said. “There are a lot of people in North Carolina who want to make their communities better places to live. There are a lot of young dentists who want to be part of a better future. We feel like we have the perfect opportunity to make ECU a pillar in this endeavor.”
The project will be based at Ross Hall with some components at the school’s community service learning center in Ahoskie and other sites around the state. During the grant’s first planning year, the team will also enlist consulting expertise from Dr. Lorrie Basnight, executive director of the Eastern Area Health Education Center and associate dean for continuing medical education at the ECU Brody School of Medicine, and Crystal Adams, program director of the Department of Dental Hygiene at Catawba Valley Community College in Hickory, N.C. Adams coordinates an online training program for community dental health coordinators (CDHCs) that prepares dental hygienists and dental assistants to work with communities to improve access to care.
The diverse team reflects the interprofessional approach of the grant itself, in the spirit of collaborating to provide more complete care to patients.
“This type of collaboration is what makes the Health Sciences Campus at ECU so unique,” Jacobs said. “While these issues are important to us all, these large endeavors are only possible when individuals with diverse abilities and expertise are able to collaborate. This type of project is important to everyone at ECU. We all want to better serve our community and provide better training for everyone moving forward.”
Preparing for an evolving health care system
The third component of the grant will work to help new dental professionals evolve along with the changing health care delivery system.
The gap for vulnerable populations is due to both gaps in Medicaid reimbursement and Medicare funding—where currently no dental benefits exist—and a shift toward an aging population.
“ECU is supporting the dental workforce transition in an emerging health care system,” Webb said. “It will no longer be acceptable to simply provide late-stage repair. A proactive approach will be necessary, especially as the demographics of the population shifts with more ‘baby boomers’ moving into an age category that is characterized by many more complex medical conditions.”
The grant will allow the team to meet these factors head-on by integrating medical, dental and societal factors that impact health care and producing professionals who can navigate the new system.
“Medically complex patients are increasingly being seen in dental offices,” Webb said. “As medical science advances more and more, patients are needing dental care that have conditions they may not have even survived a few years ago. Integration of care is essential so that there is communication among the health care providers to provide the patient the best treatment possible.”